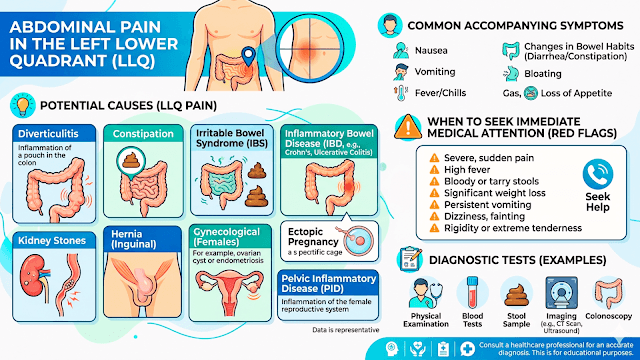
Causes, Symptoms & Treatment
Pathophysiology
Pain in the left lower quadrant (LLQ) arises from irritation, inflammation, obstruction, ischemia, or distension of structures located in or referred to the LLQ region. The sensation of pain in this region is mediated by visceral, somatic, or referred nerve pathways.
Mechanisms of Pain
- Visceral pain originates from the internal organs (e.g., sigmoid colon, ureter, ovary). These structures are innervated by autonomic afferent fibers, and the pain is typically dull, poorly localized, and colicky in nature. It results from distension, ischemia, or inflammation.
- Somatic pain arises when parietal peritoneum or abdominal wall structures are irritated. This pain is sharp, well localized, and often accompanied by guarding or rebound tenderness.
- Referred pain occurs when sensory fibers from distant organs share the same spinal segment. For example, Ureteric colic can radiate to the groin due to shared innervation (T10–L2 segments).
Nerve Pathways
- The lower thoracic (T10–T12) and lumbar (L1–L2) spinal nerves transmit afferent signals from abdominal viscera.
- Pain signals from the sigmoid colon and left ureter often converge in these spinal segments, making localization challenging.
Physiological Contributors
- Inflammation: Releases prostaglandins, bradykinin, and cytokines that sensitize nociceptors.
- Ischemia: Causes lactic acidosis and stimulation of chemoreceptors.
- Distension or obstruction: Activates stretch receptors, causing cramping pain.
Organs Involved
The left lower quadrant of the abdomen contains several visceral and vascular structures. Pain in this region can originate from one or more of the following:
| Organ/System | Relevant Conditions | Clinical Notes |
| Sigmoid Colon | Diverticulitis, volvulus, colitis, ischemia | Most common source of LLQ pain in adults; typically presents with fever, altered bowel habits, localized tenderness |
| Left Ovary & Fallopian Tube (Females) | Ovarian cyst, torsion, ectopic pregnancy, pelvic inflammatory disease (PID) | Gynecological sources often mimic intestinal pathology |
| Left Ureter | Ureteric colic due to renal stones or infection | Pain radiates to groin, may be associated with hematuria |
| Left Kidney (Lower Pole) | Pyelonephritis, hydronephrosis | Flank pain that may extend to LLQ |
| Descending Colon | Colitis, inflammatory bowel disease (IBD), malignancy | Chronic pain, often with altered bowel habits or bleeding |
| Left Iliac Vessels | Thrombosis, aneurysm (rare) | May cause dull, aching pain |
| Musculoskeletal Structures | Abdominal wall strain, hernia | Pain localized to movement or palpation |
Causes
Acute Causes
| System | Condition | Description / Key Features |
| Gastrointestinal | Diverticulitis | Inflammation of sigmoid diverticula; LLQ pain, fever, leukocytosis, and altered bowel movements |
| Infectious colitis | Caused by bacterial or viral infection; associated with diarrhea and systemic symptoms | |
| Bowel obstruction | Colicky pain, distension, vomiting; may result from adhesions, hernia, or tumor | |
| Ischemic colitis | Sudden onset pain with rectal bleeding in elderly or vascular-compromised patients | |
| Genitourinary | Ureteric colic | Sharp, radiating pain to groin; hematuria; caused by stone impaction |
| Pyelonephritis | Dull, constant pain with fever, chills, urinary frequency, and costovertebral angle tenderness | |
| Gynecological (Females) | Ovarian torsion | Sudden, severe unilateral pain; may follow cyst rupture; surgical emergency |
| Ectopic pregnancy | Lower abdominal pain, amenorrhea, and vaginal bleeding; positive pregnancy test | |
| Pelvic inflammatory disease (PID) | Bilateral lower pain, fever, discharge; often sexually transmitted | |
| Musculoskeletal | Rectus sheath hematoma | Following trauma or anticoagulation; localized pain and bruising |
Chronic Causes
| System | Condition | Description / Key Features |
| Gastrointestinal | Irritable Bowel Syndrome (IBS) | Recurrent pain with bowel habit changes; relieved by defecation |
| Chronic diverticular disease | Recurrent LLQ discomfort post-diverticulitis; bloating, constipation | |
| Colorectal cancer | Progressive, dull pain; change in bowel habits, blood in stool | |
| Genitourinary | Chronic Pyelonephritis | Recurrent flank pain, low-grade fever, dysuria |
| Gynecological | Endometriosis | Cyclical LLQ pain, Dysmenorrhea, infertility |
| Ovarian cyst (benign) | Dull, intermittent pain or fullness sensation | |
| Musculoskeletal | Hernia, muscle strain | Exacerbated by activity; palpable tenderness |
Line of Management
Initial Assessment
History
· Onset, duration, character, and radiation of pain.
· Associated symptoms: nausea, bowel changes, urinary complaints, menstrual history (in females).
Physical Examination
· Inspection, palpation (guarding, rebound), percussion, and auscultation.
· Digital rectal and pelvic exams if indicated.
Diagnostic Evaluation
| Test | Purpose / Findings |
| Complete blood count (CBC) | Leukocytosis in infection/inflammation |
| Urinalysis | Detects hematuria, infection (for ureteric causes) |
| Serum electrolytes, renal function tests | Evaluate dehydration, renal impairment |
| β-hCG (in females) | Exclude ectopic pregnancy |
| Abdominal ultrasound | First-line for gynecological or urinary causes |
| CT abdomen and pelvis (contrast-enhanced) | Gold standard for diverticulitis, obstruction, abscess |
| Colonoscopy | For chronic pain, IBD, or malignancy suspicion |
| Pelvic MRI | For detailed gynecological or soft tissue pathology |
Line of Management
Medical Management
Diverticulitis: Broad-spectrum antibiotics (e.g., ciprofloxacin + metronidazole), bowel rest, fluids.
· Ureteric colic: NSAIDs, hydration, alpha-blockers (tamsulosin), lithotripsy if indicated.
· PID / Endometriosis: Antibiotics, hormonal therapy, or laparoscopic management.
· IBS: Dietary modification, probiotics, antispasmodics.
· Colitis: Antibiotics (if bacterial), corticosteroids or aminosalicylates for IBD.
Surgical Management
· Perforated diverticulitis / abscess: Hartmann’s procedure or drainage.
· Ovarian torsion / ectopic pregnancy: Emergency surgery.
· Obstruction or malignancy: Resection, stenting, or bypass.
Follow-up Care
- Lifestyle modification: High-fiber diet, adequate hydration, regular exercise.
- Surveillance colonoscopy for chronic diverticular disease or post-malignancy.
- Regular imaging for renal stones or cyst recurrence.
- Patient education on warning signs (fever, severe pain, rectal bleeding).
Summary
Pain in the left lower quadrant is a multifactorial clinical presentation requiring a methodical diagnostic approach. The most common cause in adults is sigmoid diverticulitis, while in women of reproductive age, gynecological causes such as ovarian torsion or ectopic pregnancy must be urgently ruled out. A combination of thorough history-taking, focused physical examination, and targeted imaging ensures timely diagnosis and appropriate management, minimizing complications.
Disclaimer: The information provided in this blog post is for educational and informational purposes only and should not be considered medical advice. It is not intended to replace professional medical consultation, diagnosis, or treatment. Always seek the guidance of a qualified healthcare professional regarding any medical condition or health-related concerns. The author and publisher are not responsible for any actions taken based on the information presented in this article.