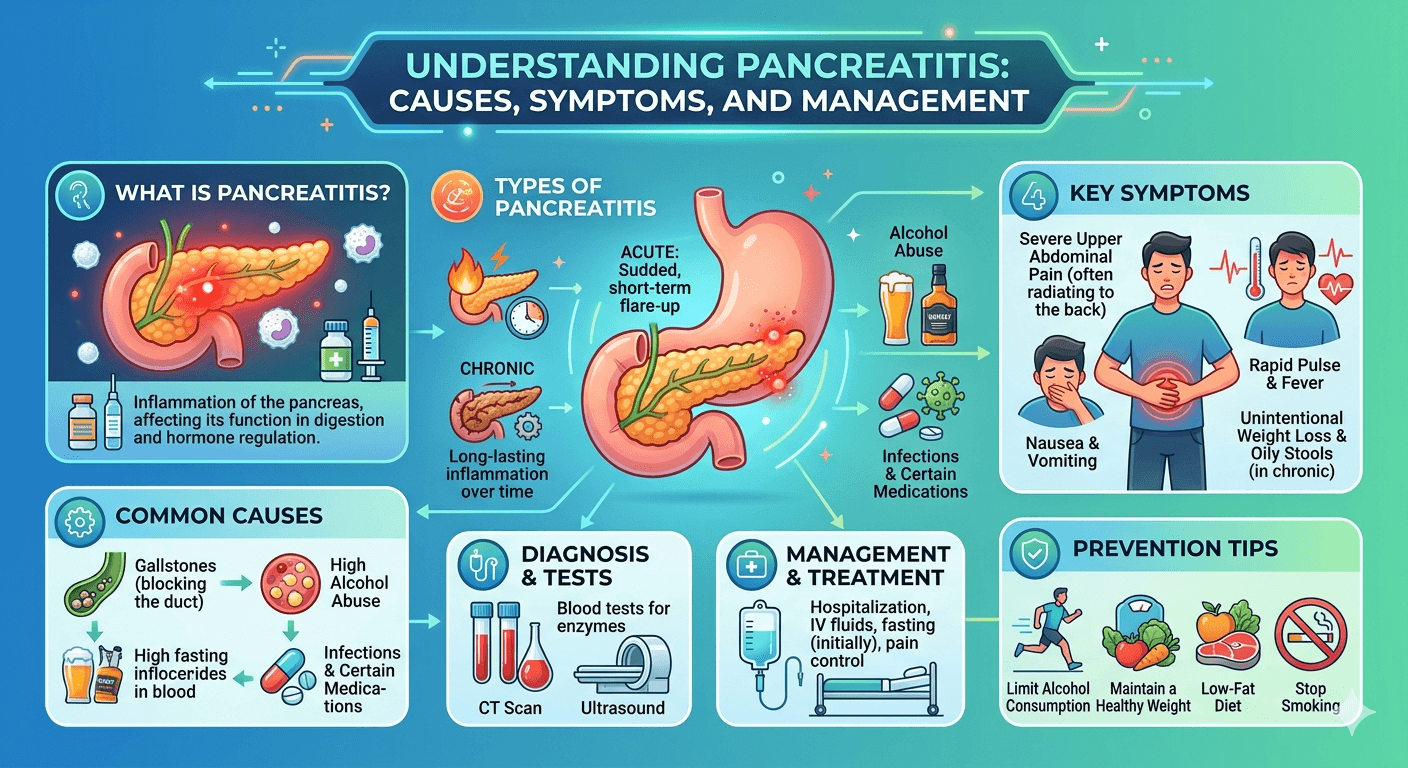
Introduction
Pancreatitis is an inflammatory condition of the pancreas that can present as either an acute or chronic disease. The pancreas is an important organ located behind the stomach and plays a major role in digestion and blood sugar regulation. It produces digestive enzymes that help break down fats, proteins, and carbohydrates, while also secreting hormones such as insulin and glucagon that regulate glucose metabolism.
Pancreatitis occurs when digestive enzymes become activated inside the pancreas instead of the small intestine, leading to self-digestion and inflammation of pancreatic tissue. The condition can range from mild inflammation that resolves with supportive care to severe life-threatening disease associated with organ failure and systemic complications.
Acute pancreatitis develops suddenly and may resolve completely with appropriate treatment, whereas chronic pancreatitis is characterized by long-term inflammation that causes irreversible structural damage and progressive loss of pancreatic function.
Understanding the causes, pathophysiology, clinical features, diagnosis, and management of pancreatitis is essential for early recognition and prevention of complications.
Pathophysiology of Pancreatitis
The fundamental mechanism in pancreatitis involves premature activation of pancreatic digestive enzymes within the pancreatic tissue. Under normal conditions, digestive enzymes are synthesized in inactive forms and become activated only after reaching the duodenum. In pancreatitis, this protective mechanism fails.
Enzyme Activation and Autodigestion
Premature activation of trypsin inside pancreatic acinar cells initiates a cascade of enzyme activation. Activated enzymes digest pancreatic tissue, resulting in:
- Cellular injury
- Fat necrosis
- Hemorrhage
- Edema
- Inflammatory response
This process is known as Autodigestion of the pancreas.
Inflammatory Response
Inflammatory mediators such as cytokines and chemokines are released during pancreatic injury. These substances attract inflammatory cells and amplify tissue damage. Severe inflammation may extend beyond the pancreas and produce systemic inflammatory response syndrome (SIRS).
Microcirculatory Disturbance
Inflammation leads to vascular permeability, edema, and impaired blood flow within the pancreas. Reduced perfusion can result in ischemia and pancreatic necrosis.
Systemic Effects
In severe cases, inflammatory mediators enter systemic circulation and may affect multiple organs, causing:
- Acute respiratory distress syndrome (ARDS)
- Acute kidney injury
- Shock
- Sepsis
- Multi-organ failure
Chronic Pancreatitis
Repeated episodes of inflammation cause fibrosis, calcification, and destruction of pancreatic tissue. Over time, the pancreas loses both exocrine and endocrine functions, leading to malabsorption and diabetes mellitus.
Causes of Pancreatitis
Pancreatitis has multiple etiologies. The most common causes differ between acute and chronic forms.
Common Causes of Acute Pancreatitis
Gallstones
Gallstones are among the leading causes of acute pancreatitis. Small stones may obstruct the pancreatic duct or ampulla of Vater, causing reflux and enzyme activation.
Alcohol Consumption
Excessive alcohol intake directly damages pancreatic acinar cells and increases the viscosity of pancreatic secretions, contributing to ductal obstruction and inflammation.
Hypertriglyceridemia
Very high triglyceride levels can trigger pancreatic inflammation due to toxic free fatty acid production.
Medications
Certain drugs are associated with pancreatitis, including:
- Azathioprine
- Valproic acid
- Thiazide diuretics
- Corticosteroids
- Didanosine
Infections
Viral infections such as mumps, hepatitis viruses, and cytomegalovirus may cause pancreatic inflammation.
Trauma
Abdominal trauma and surgical procedures can injure pancreatic tissue.
ERCP
Pancreatitis is a recognized complication of ERCP(Endoscopic Retrograde Cholangiopancreatography)
Autoimmune Disorders
Autoimmune pancreatitis results from immune-mediated inflammation.
Metabolic Causes
- Hypercalcemia
- Genetic mutations
- Obesity
Idiopathic Causes
In some patients, no definite cause is identified.
Causes of Chronic Pancreatitis
- Chronic alcohol abuse
- Smoking
- Genetic disorders
- Autoimmune pancreatitis
- Recurrent acute pancreatitis
- Obstructive pancreatic duct disease
Signs and Symptoms of Pancreatitis
The clinical presentation depends on the severity and duration of inflammation.
Symptoms of Acute Pancreatitis
Abdominal Pain
Severe epigastric pain is the hallmark symptom. The pain often:
- Radiates to the back
- Begins suddenly
- Worsens after meals
- Improves slightly when leaning forward
Nausea and Vomiting
Persistent nausea and repeated vomiting are common.
Fever
Inflammation and infection may produce fever.
Abdominal Tenderness
The abdomen may be tender and distended.
Loss of Appetite
Patients often avoid eating because it worsens pain.
Tachycardia and Hypotension
Severe cases may lead to dehydration and shock.
Severe Clinical Features
- Respiratory distress
- Cyanosis
- Altered mental status
- Jaundice
- Multi-organ dysfunction
Signs of Chronic Pancreatitis
Chronic Abdominal Pain
Pain may be recurrent or persistent.
Malabsorption
Insufficient digestive enzyme production leads to:
- Steatorrhea
- Weight loss
- Nutritional deficiencies
Diabetes Mellitus
Destruction of insulin-producing cells may cause secondary diabetes.
Pancreatic Calcification
Calcifications may be visible on imaging studies.
Diagnosis of Pancreatitis
Diagnosis is based on clinical findings, laboratory investigations, and imaging studies.
Diagnostic Criteria for Acute Pancreatitis
Diagnosis is usually confirmed when at least two of the following are present:
- Characteristic abdominal pain
- Elevated pancreatic enzymes
- Imaging findings suggestive of pancreatitis
Laboratory Investigations
Serum Amylase and Lipase
Lipase is more specific and remains elevated longer than amylase.
Complete Blood Count (CBC)
May show elevated white blood cell count.
Liver Function Tests
Abnormal liver enzymes may suggest gallstone pancreatitis.
Serum Calcium and Triglycerides
Used to identify metabolic causes.
Blood Glucose
Hyperglycemia may occur due to endocrine dysfunction.
C-Reactive Protein (CRP)
Helps assess severity of inflammation.
Imaging Studies
Ultrasound Abdomen
Useful for detecting gallstones and biliary obstruction.
Contrast-Enhanced CT Scan
CT scan is important for assessing:
- Pancreatic inflammation
- Necrosis
- Fluid collections
- Complications
MRI and MRCP
Helpful in evaluating pancreatic ducts and soft tissues.
Endoscopic Ultrasound (EUS)
Useful for detecting small gallstones and structural abnormalities.
Severity Assessment
Several scoring systems are used to predict severity:
- Ranson criteria
- APACHE II score
- BISAP score
- Glasgow score
Line of Management of Pancreatitis
Management depends on the severity, cause, and complications.
Initial Management of Acute Pancreatitis
Fluid Resuscitation
Aggressive intravenous hydration is essential to maintain organ perfusion and prevent complications.
Pain Management
Analgesics are administered to control severe abdominal pain.
Nutritional Support
Early enteral feeding is preferred over prolonged fasting. Severe cases may require nasojejunal feeding.
Bowel Rest
Temporary restriction of oral intake may be necessary during severe attacks.
Oxygen Therapy
Provided when respiratory compromise occurs.
Treatment of Underlying Causes
Gallstone Pancreatitis
- ERCP for biliary obstruction
- Cholecystectomy to prevent recurrence
Alcohol-Induced Pancreatitis
Complete abstinence from alcohol is critical.
Hypertriglyceridemia
- Insulin therapy
- Lipid-lowering agents
- Plasmapheresis in severe cases
Antibiotics
Routine prophylactic antibiotics are not recommended. Antibiotics are reserved for infected necrosis or confirmed infections.
Management of Complications
Pancreatic Necrosis
May require drainage or surgical intervention.
Pancreatic Pseudocyst
Large or symptomatic pseudocysts may need endoscopic or surgical drainage.
Organ Failure
Intensive care support may be required for respiratory, renal, or circulatory failure.
Management of Chronic Pancreatitis
Lifestyle Modifications
- Alcohol cessation
- Smoking cessation
- Dietary modification
Pancreatic Enzyme Replacement Therapy
Improves digestion and reduces steatorrhea.
Diabetes Management
Insulin therapy may be necessary.
Pain Control
Pain management may include:
- Analgesics
- Nerve blocks
- Endoscopic therapy
- Surgery in selected cases
Surgical Management
Surgery may be indicated for:
- Duct obstruction
- Severe pain
- Complications
- Suspicion of malignancy
Prognosis of Pancreatitis
The prognosis depends on disease severity, complications, and underlying cause.
Acute Pancreatitis
Most cases are mild and resolve completely with supportive care. However, severe acute pancreatitis can carry significant mortality due to:
- Pancreatic necrosis
- Sepsis
- Multi-organ failure
Early diagnosis and aggressive treatment improve outcomes.
Chronic Pancreatitis
Chronic pancreatitis is progressive and irreversible. Long-term complications include:
- Chronic pain
- Malnutrition
- Diabetes mellitus
- Pancreatic insufficiency
- Increased risk of pancreatic cancer
Lifestyle modifications and regular follow-up can improve quality of life and reduce complications.
Prevention of Pancreatitis
Several preventive strategies may reduce the risk of pancreatitis.
Lifestyle Measures
- Avoid excessive alcohol intake
- Stop smoking
- Maintain healthy body weight
- Follow a balanced low-fat diet
Control of Metabolic Disorders
- Manage triglyceride levels
- Treat hypercalcemia
- Control diabetes mellitus
Gallstone Prevention
Early management of gallstones can reduce the risk of biliary pancreatitis.
Medication Monitoring
Patients taking high-risk medications should be monitored for pancreatic side effects.
Conclusion
Pancreatitis is a potentially serious inflammatory disease of the pancreas that can occur in acute or chronic forms. Gallstones and alcohol abuse remain the most common causes, although metabolic disorders, medications, infections, and autoimmune diseases may also contribute.
Patients commonly present with severe abdominal pain, nausea, vomiting, and systemic symptoms. Early diagnosis through laboratory tests and imaging studies is important for timely management and prevention of complications. Supportive care, fluid resuscitation, nutritional support, and treatment of underlying causes form the cornerstone of therapy.
Improved awareness, early intervention, and long-term lifestyle modifications are essential for better outcomes and improved quality of life in patients with pancreatitis.